Analyst Insight: The battle between fructose and glucose

Sugar continues to be a hot topic when it comes to nutrition, with its excessive consumption being blamed for the steep rise in the level of overweight and obese individuals globally and the resulting health complications.
However, manufacturers’ focus should not be on reducing or replacing fructose sugars with glucose sugars, rather focus on reducing overall use and reliance on sugar. While health concerns connected to high fructose corn syrup (HFCS) should start to disperse as newer research invalidates adverse effects of fructose on health compared to glucose
Fructose targeted
Although not proven, fructose and fructose-containing sugars; in particular HFCS has been accused of being more detrimental to an individual’s health than glucose and glucose-containing sugars.
Fructose is a naturally occurring monosaccharide sugar, found in fruits, some vegetables and honey. Being the sweetest natural sugar, it is only present in very small amounts naturally. Much of the concerns around HFCS are linked to the increasing amounts consumed in modern western diets.
With HFCS now a common ingredient in processed foods, we no longer just eat small quantities found in natural sources.
HFCS free
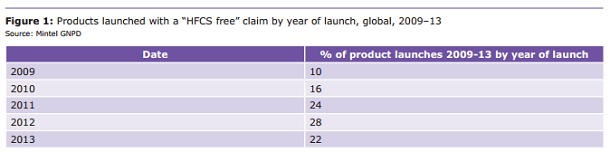
In response advertising the fact that products are free from HFCS has become more common over the past five years, although launches of “HFCS free” products dipped slightly in 2013.
The use of “HFCS free” claims appeals to those consumers actively trying to avoid HFCS. This includes more than one third of US respondents who consider no HFCS claims important when purchasing non-alcoholic drinks and almost three in 10 US respondents who use low-/no-calorie sugar substitutes to avoid HFCS.
Metabolic differences?
HFCS’s bad reputation stems from biochemical differences between glucose and fructose. Despite fructose and glucose holding the same calorific values, the two sugars are processed differently in the body, causing different responses on ingestion.
Consequently HFCS has been linked to fuelling the obesity epidemic, with its rising usage in processed foods since the 1980s tracking the upward trajectory of obesity.
Fructose is poorly absorbed from the gastrointestinal tract and is almost entirely metabolised by the liver. Whereas glucose, the body’s preferred source of energy, is metabolised within the gastrointestinal tract, entering the bloodstream almost immediately causing blood sugars to rise and in response the body releases insulin to help normalise blood sugar levels.
Glucose molecules bind to the insulin and are transported to cells that need extra energy, any unused glucose is deposited in fat cells, stored as fat. In comparison fructose does not stimulate the release of insulin, as it is processed in the liver. When too much fructose enters the liver, the liver cannot always process it fast enough for the body to use it as sugar, so instead it is converted into glycerol, a key component of triglycerides.
This has been suggested as inadvertently raising the level of free triglycerides in the blood, a key risk factor for heart disease.
It has also been suggested that the different metabolic process fructose follows means it evades the normal appetite signalling system, by not stimulating the release of insulin and other key appetite regulating hormones like leptin.
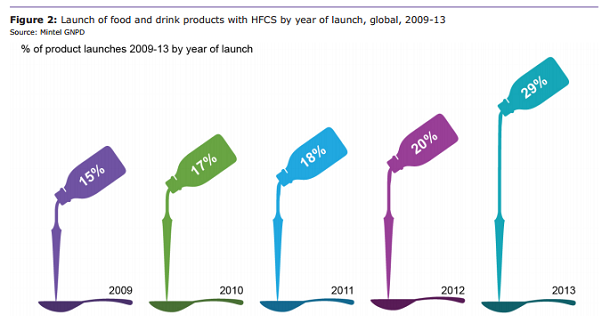
Despite the somewhat negative image of HFCS, it is still used extensively in the food industry to reduce or replace sugar, and typically offers a cost saving and extended shelf life. This is reflected by its increasing use in food and drink launches globally in recent years.
Replacing fructose with glucose sugars is not the answer
However, evidence supporting the proposition that the metabolic differences between glucose and fructose means fructose is more detrimental to one’s health than glucose is so far inconclusive.
A recent study published in the Current Opinion in Lipidology journal looked further into the metabolic differences between fructose and glucose by assessing the effect isocaloric replacement of glucose with fructose has on cardiometabolic risk factors.
The study found that consuming fructose in place of glucose can in fact increase total cholesterol and postprandial triglycerides in some cases, but on the other hand fructose did not affect insulin production, other fat levels in the blood stream or makers of fatty liver disease any more than glucose did. It also reported that fructose may actually hold some advantages over glucose including being better at promoting healthy body weight, blood pressure and glycaemic control.
However, the research admits that there are some limitations in the data and to address some of the remaining uncertainties, larger, longer and high quality ‘real world’ trials are required.
The real focus should not be on replacing fructose in the diet with glucose, rather shifting attention to limiting and reducing the consumption of all highly refined carbohydrates.
Based in the London office, Laura Jones joined Mintel as a Global Food Science Analyst in 2012. Laura holds a Bachelor of Science, with a major in Food Science and Nutrition, along with a Post Graduate Diploma in Bioscience Enterprise. Prior to her role at Mintel, she worked in the refrigeration and cooking division of a New Product Development Team for an appliance company in New Zealand. ywbarf@zvagry.pbz